Gluten, Brain Health, and Neurological Disparities
We are here to talk about a powerful act of kindness you can give yourself: protecting your brain through simple food choices. Food is more than fuel. Every bite sends signals to your body’s control center, the brain.
Today, we are focusing on gluten, a protein found in wheat, barley, and rye. For many people, gluten is harmless. But for others, especially people with celiac disease or gluten sensitivity, it may trigger inflammation that can affect the gut, immune system, and brain.
How Gluten May Affect The Brain
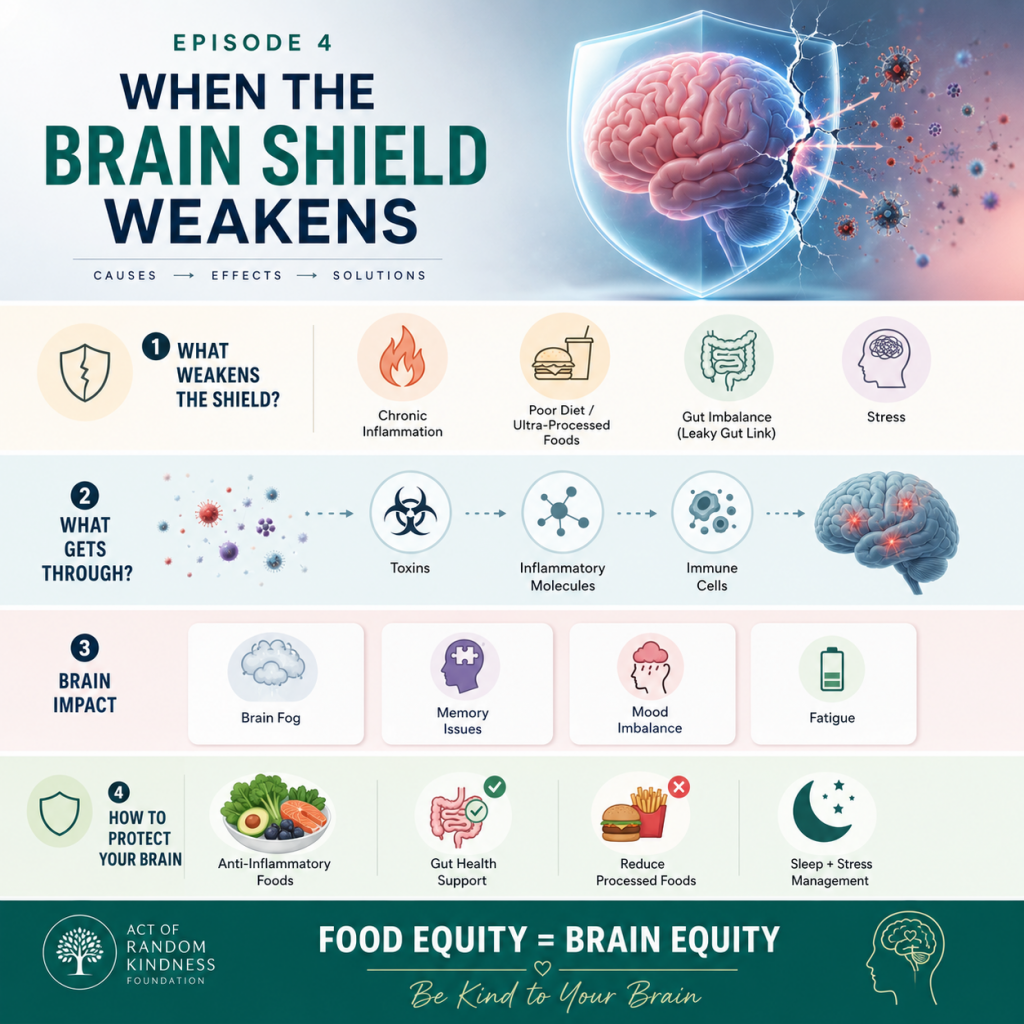
The first place gluten can cause problems is often the gut. In some sensitive people, gluten may increase intestinal permeability, sometimes called “leaky gut,” which means the gut lining becomes more permeable than it should be. When that happens, unwanted particles may enter the bloodstream and trigger an immune response.
That immune response can create chronic inflammation. Research shows that gluten-related disorders can be linked to neurological and psychiatric symptoms, including brain fog, headaches, mood changes, cognitive problems, and depression. Inflammation may also affect the blood-brain barrier, which is the brain’s protective shield, and allow inflammatory signals to irritate brain tissue.
Why This Matters For Neurological Disparities
Neurological disparities are unfair differences in brain health between groups of people. These differences can be shaped by income, access to care, nutrition knowledge, and whether people are able to get tested for conditions like celiac disease or gluten sensitivity.
This matters because some people can quickly identify food triggers and make changes, while others may go years without answers. People with less access to healthcare or nutrition support may be more likely to live with untreated inflammation, ongoing brain fog, migraines, fatigue, or mood symptoms. That can widen the gap in brain health over time.
Supporting Evidence
Research from NIH and other medical sources shows a real connection between gluten-related disorders and the nervous system. A review in PMC found that neurological manifestations in celiac disease can include ataxia, peripheral neuropathy, headaches, cognitive impairment, and depression. Another review noted that gluten may contribute to neurodegeneration in susceptible people through inflammatory and immune pathways.
It is also important to be clear: gluten does not harm everyone in the same way. The strongest evidence is for people with celiac disease and some people with non-celiac gluten sensitivity. For those individuals, removing gluten can improve symptoms and support overall health.
A Brain-Kind Approach
A brain-supportive lifestyle usually means paying attention to how food makes you feel. If someone has ongoing headaches, brain fog, fatigue, anxiety, or memory issues after eating gluten, it may be worth discussing testing or a supervised diet change with a clinician.
For people who need to avoid gluten, a balanced diet can still include vegetables, fruits, beans, nuts, eggs, fish, meat, gluten-free whole grains, and healthy fats. The goal is not restriction for its own sake. The goal is to reduce inflammation and protect brain health.
Conclusion
Being kind to your brain means listening to it. For some people, gluten may be more than a digestive issue — it may be part of a bigger inflammation story that affects thinking, mood, and memory. When access to diagnosis and healthy food is unequal, those brain effects can become part of a larger neurological disparity.
Resources
- NIH/PMC: Celiac Disease and Neurological Manifestations: From Gluten to the Brain
- NIH/PMC: Gluten, Inflammation, and Neurodegeneration
- NIH/PMC: The Neuropathology of Gluten-Related Neurological Disorders
- NIH/PMC: Neurologic and Psychiatric Manifestations of Celiac Disease and Gluten Sensitivity
- NIH/PMC: Intestinal Permeability and its Regulation by Zonulin
- NIH/PMC: All disease begins in the (leaky) gut: role of zonulin-mediated intestinal permeability
- Celiac Disease Foundation: Brain Images Show Effects of Celiac Disease
